 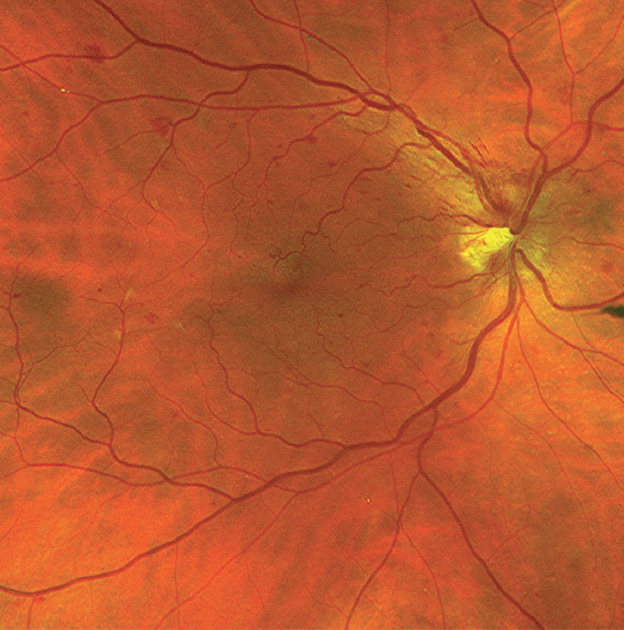
Microaneurysms have also been reported in leukemia and plasma cell dyscrasias. They are classically seen in the posterior fundus in diabetic retinopathy. Microaneurysms are small outpouchings in the retinal capillary wall that appear as tiny red dots in the retina on ophthalmoscopic examination. However, Keresh et al 20 noted no correlation with presence of retinopathy and hematocrit and white blood cell counts in patients with myeloid leukemia. The same authors reported a higher median white blood cell count in patients with intraretinal hemorrhages than in those without intraretinal hemorrhages and concluded that a high white blood cell count may be at least as important as anemia and thrombocytopenia in the pathogenesis of retinopathy in acute leukemia. 1 On the contrary, Jackson et al 19 found no association between intraretinal hemorrhages and the hemoglobin level or platelet count in 63 newly diagnosed acute leukemia patients. 18 Finally, in a study of 226 patients, retinal hemorrhages were seen in all patients with both severe anemia and severe thrombocytopenia. 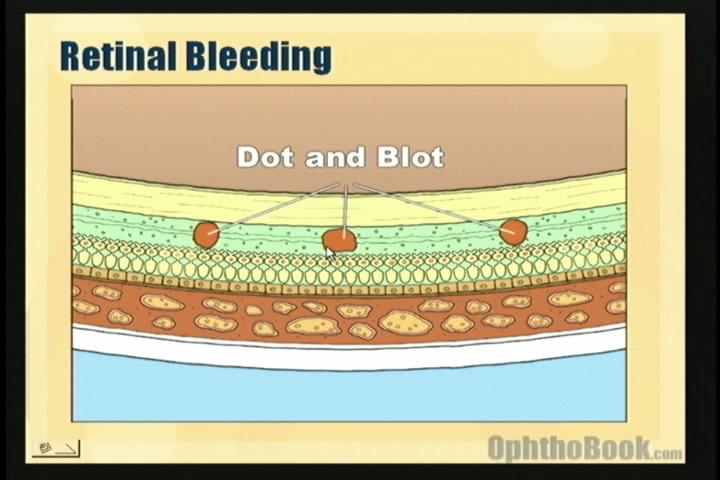
Additionally, in a study of 41 patients with myelodysplastic syndrome (a group of preleukemic disorders) retinal hemorrhage significantly depended on platelet count. Consistent with this observation, Reddy and Jackson 17 -in a study of 127 patients with acute leukemia-found that intraretinal hemorrhages were significantly associated with high white count and low platelet count. In a prospective study of 117 patients with acute leukemia, Guyer et al 16 reported that thrombocytopenia is the most important factor in the pathogenesis of intraretinal hemorrhages. In a study of 152 patients with various blood diseases, Holt and Gordon-Smith 8 reported that retinal hemorrhages in leukemic patients were observed most frequently when severe anemia, severe thrombocytopenia, or a high percentage of circulating blast cells were also present. In a study of 67 patients with anemia and/or thrombocytopenia, Rubenstein et al 15 found that retinal hemorrhage is much more likely to occur when anemia is accompanied by thrombocytopenia than when either is present alone. 7 The red center is blood, which may be associated with a cotton-wool spot (CWS) or a leukemic retinal infiltrate. 18-6) or more commonly a platelet-fibrin thrombus. The white center may be associated with a leukemic embolus ( Fig. 18-5) may be seen in the retinae of patients with a blood dyscrasia. 18-1) and, much less commonly, red-centered infiltrates ( Fig. These large superficial retinal hemorrhages may break through the ILM and extend into the vitreous cavity ( Fig. Large blot or boat-shaped hemorrhages may be observed and are present beneath the internal limiting membrane (ILM) of the retina (i.e., sub-ILM hemorrhage) ( Fig. Flame-shaped hemorrhages are located in the nerve fiber layer of the retina, and dot-blot hemorrhages are typically located in the inner nuclear and outer plexiform layers ( Fig. Flame-shaped and dot-blot hemorrhages are the most commonly encountered intraretinal hemorrhages in blood dyscrasias ( Fig. Retinal hemorrhages may take various configurations based on their location within the retina. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
